Alumni Profile
 Gerald Thomson’96
Gerald Thomson’96Gerald Thomson, MD, who received an honorary VP&S degree in 1996, is the Samuel Lambert Professor Emeritus of Medicine and the Robert Sonneborn Professor Emeritus of Medicine at VP&S. His 48 years as a member of the Columbia faculty have involved a range of local and national commitments and efforts including as a clinician, teacher, and director of a maintenance dialysis program. He also has been an advocate for justice and human rights in health and health care, director of medicine at Harlem Hospital Center, chief medical officer and executive vice president for professional affairs at the former Columbia-Presbyterian Medical Center, senior associate dean at what is now VP&S, chair of the American Board of Internal Medicine, and president of the American College of Physicians. He has addressed disparities in health and health care and reviewed the involvement of physicians in the interrogation and torture of post 9/11 U.S. detainees.
Dr. Thomson reflected on the highlights of his long career in two interviews conducted in April 2018.
From Harlem to Howard
Born at the Women’s and Children’s Pavilion at the Presbyterian Hospital to immigrant parents from Jamaica, Gerald Thomson grew up as a young child in Harlem and Washington Heights. The family saw the “Medical Center” and its Vanderbilt Clinic as their “doctor.” Later, he had part-time jobs after school throughout high school and college to help the family make ends meet. In 1952, he returned to Queens College after military service and continued working at outside jobs. He was determined to become a doctor “for as long as I could remember.”
Despite the impact of the outside work on his grades, he thought he had done well enough to get into medical school, but he faced discouragement of other kinds. A college faculty member told him: “You colored boys always want to be doctors. You’d be better off if you joined the plumbers’ union.”
“I never forgot those words,” Dr. Thomson still winces at the sting of the memory. “Today I call it negative mentoring. It made me angry, and all the more determined.”
Of the 17 American medical schools to which he applied, he was admitted to two, Howard University’s medical school in Washington, D.C., and Meharry Medical College in Nashville, both historically African-American schools. “There have often been thoughts that if it had not been for Howard and Meharry, how many would not have had the opportunity to care for patients in their communities, to contribute leadership and advocacy,” Dr. Thomson says. He ultimately chose to attend Howard partly because one of his part-time jobs, as a Red Cap at Grand Central Station, allowed him to become a member of the railroad union so he could travel free between New York and Washington, but not to Nashville. “It was a matter of carfare,” he says.
“At medical school,” Dr. Thomson recalls,” I was not working at an outside job for the first time since high school, so I could devote myself entirely to learning. It was a great privilege.”
Performing at the top of his class, he earned a full scholarship and came to the attention of William Hawthorne, MD, PhD, the preeminent chair of physiology, who invited him to participate in research.
Dr. Thomson says his greatest benefit from Howard came when he was registering for his sophomore year and met a freshman, Carolyn Webber. He carried her books home. They have been carrying each other’s books ever since, through 60 years of marriage. Dr. Webber is now a retired professor of pathology.
Dr. Thomson’s completion of residency and fellowship training in nephrology with Dr. Eli Friedman at State University of New York’s Downstate Medical Center-Kings County Hospital in Brooklyn coincided with stunning developments in the treatment of end-stage kidney failure. The development of safe, repeated access to patients’ circulating blood made it possible for patients with terminal renal failure to receive dialysis to maintain reasonable health for months or years. Dr. Thomson spent time with Dr. Belding Scribner and his group at the University of Washington in Seattle to observe the new techniques and the beginnings of maintenance dialysis treatment. He returned to Brooklyn and with Dr. Friedman set up and directed what became one of the nation’s earliest and largest dialysis programs.
“It was like suddenly having a treatment for terminal cancer,” he remembers. He was greatly stirred by “the drama of seeing patients otherwise doomed to die with the diagnosis of chronic renal failure pull through, thanks to the intervention. We had the ability to resurrect those patients and give them life for months or years. We ultimately set up a huge ward, with 14 patients hooked up to a single dialysate-producing pump, being treated at the same time. We were also able to help other regional centers get started as quickly as possible.” The latter was particularly important as Dr. Thomson experienced the realities of not having enough dialysis facilities and the anguish of rationing in medicine.
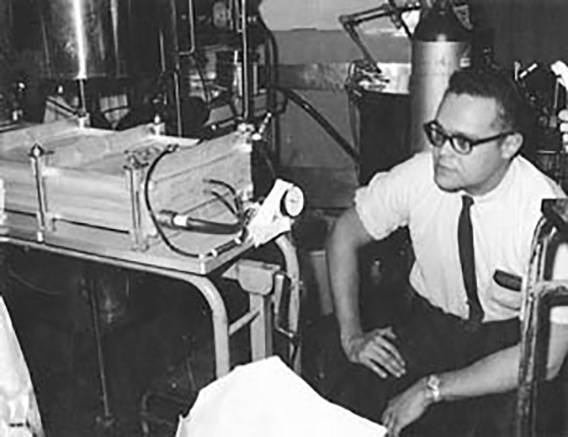 Dr. Thomson with artificial kidneys at Kings County Hospital in 1965
Dr. Thomson with artificial kidneys at Kings County Hospital in 1965While at Kings County, Dr. Thomson witnessed glaring disparities in health care because of the lack of resources at public hospitals compared to well-funded private institutions. He later joined forces with a colleague, Dr. Seymour Glick, to co-found the Society of Urban Physicians, an organization of several hundred public hospital senior physicians who advocated for improved conditions in New York’s public hospitals. The group gathered information, held press conferences, and issued reports. They also organized a national conference on public general hospitals.
In 1968, the city government instructed Columbia University to move its illustrious First Medical Division, headed by Dr. Charles Ragan, from Bellevue to Harlem Hospital as part of an overall plan to improve staffing and professional services through funded affiliation contracts that made universities and their medical schools responsible for professional services in the public hospitals. Two years later, Dr. Ragan recruited Dr. Thomson to join the Columbia faculty and set up a kidney unit in Harlem, where renal failure was widespread due in large part to the unchecked incidence of high blood pressure and diabetes. But no sooner did Dr. Thomson get things going, battling with city and state authorities to give him the four artificial kidneys and other resources he had been promised, when, in 1972, Dr. Ragan was appointed chair of the Department of Medicine at Columbia. He urged Dr. Thomson to take on direction of the Department of Medicine at Harlem. “I said I would do it for a couple of years to get things established. Fifteen years later…”
At the Medical Helm in Harlem
From 1971 to 1985, with scarce resources and against almost insurmountable community health status challenges, including poverty and the now clearly recognized effects of other social determinants of health, says Dr. Thomson, he developed a full-service Department of Medicine with 40 full-time faculty members, 120 residents and fellows, divisions in all subspecialties, fully accredited residency and fellowship training, teaching of Columbia students, and research programs.
Dr. Thomson noted: “Harlem Hospital suffered the same budgetary and resource problems that affected many publicly funded hospitals across the country. Advocacy and often activism by hospital health professionals and the informed, determined community were necessary to deal with repeated attempts to reduce funding and deny requests for needed services, equipment, and resources. Because of the affiliation contract, Columbia University became an advocate for Harlem Hospital at the highest levels, advocating for proper support of the hospital and its health professionals in keeping with the stipulated responsibilities of the contract.”
For a whole generation of black physicians who trained at Harlem Hospital, he exemplified what it meant to be a physician dedicated to community.
Dr. Thomson lauds the members of his house staff. “Absolutely committed to caring for their patients, the Harlem house staff were as good as any you could find anywhere,” he recalls, “often thinking and acting out of the box. They brought the sense of justice and activism of the times with them to Harlem. They were embraced by the community’s activism on behalf of the hospital.”
Former medical resident and immediate past NYC Commissioner of Health, Mary Bassett’79, still remembers the dire conditions and the director’s leadership style: “We lacked supplies, we had very sick patients, the operating room would be shut down because they didn’t have air conditioning, and I remember the night they ran out of respirators. But in spite of those daunting conditions, Dr. Thomson inspired us all by his example, generating standards, demanding quality of care, and commanding respect. For a whole generation of black physicians who trained at Harlem Hospital,” she added, “he exemplified what it meant to be a physician dedicated to community. He was one of that handful of people who generate standards around them.”
 Brenda Aiken’81 with Dr. Thomson, the man nicknamed "JET"
Brenda Aiken’81 with Dr. Thomson, the man nicknamed "JET"Another former resident, Brenda Aiken’81, assistant clinical professor of medicine at VP&S, director of medical services at Columbia’s student health service, and a past president of the P&S Alumni Association, recalls: “He was affectionately called the ‘JET,’ because of his initials, G-E-T, and because of his way of demanding excellence and asking probing detailed, knowledge-based questions at morning report or chief of service rounds. You had better know the reason for high anion gap metabolic acidosis or have TB in your differential diagnosis of pneumonia, as well as consider all the psychosocial and economic determinants of health. Harlem is where we went to learn urban medicine, to become advocates for communities.”
Dr. Thomson called public attention to the high death rates and poor health indices in central Harlem. Federal funding was provided to establish the Harlem primary care network, still functioning today as the Harlem Renaissance Network.
Dr. Thomson felt strongly that programs to prevent disease should also be instituted. He wrote a detailed proposal asking that a division of preventive medicine be added to the Department of Medicine.
“But when I talked about prevention, people thought I was crazy,” he says. And when he pitched the hospital administration to add a division of prevention to the Department of Medicine, he was told, “Dr. Thomson, we don’t get paid for preventing illness, we are reimbursed for treating patients.”
The indefatigable Dr. Thomson took matters in his own hands. He organized, among other initiatives, a program that trained nurses to screen thousands of people in Harlem for high blood pressure and refer those found to have hypertension to a special Harlem Hospital clinic where they were treated by the specially trained and supervised nurses.
Later, as senior associate dean at Columbia, he teamed up with the late Allan G. Rosenfield’59, former dean of the Mailman School of Public Health at Columbia, to create at Harlem Hospital the Harlem Center for Health Promotion and Disease Prevention funded by the CDC. Dr. Bassett, who went on to become the New York City health commissioner, served for a time as medical director.
The Call to Columbia-Presbyterian
In 1985, Tom Morris’58, then newly appointed president of Presbyterian Hospital, recruited Dr. Thomson to fill the position of chief medical officer and executive vice president for professional affairs to oversee the management of all professional staff and programs.
In addition, on behalf of Presbyterian Hospital, Dr. Thomson established and was president of the Washington Heights-Inwood Ambulatory Care Network (now the ACNC Ambulatory Care Network), a system of primary care centers, including medicine, pediatrics, and OB/GYN services, and some with dental units, all linked to Presbyterian Hospital. He also championed and established a special arrangement between the hospital and qualified community doctors, granting them a limited attending status that allowed them to confer with Columbia faculty, refer patients for admission, and receive coordinated information when their patients were discharged.
Also, on behalf of Presbyterian Hospital and at the request of the state, Dr. Thomson wrote and negotiated an affiliation contract between Helen Hayes Hospital, a Columbia affiliate that specializes in physical rehabilitation, and Presbyterian Hospital, adding the involvement of several additional patient care services to the rehabilitation facility.
 As senior associate dean in 1992
As senior associate dean in 1992Senior Associate Dean: Championing the Recruitment of Minority Medical Students at VP&S and other Efforts
In 1991 Dr. Thomson was appointed senior associate dean at VP&S, a position he held with distinction until 2002. Foremost among his missions were the recruitment, support, and advisement of minority medical students who were underrepresented in medicine. He became personally involved with the admissions process, helping to screen and interview applicants and working with the Admissions Committee. He also advised admitted students, sought scholarship support, and established special programs that provided experiences and advisement for college and high school students. He visited and spoke at numerous colleges and universities, often serving as an adviser to individual students and organizations. He regularly worked with the Association of American Medical Colleges to develop programs to improve the pipeline of qualified students to medical schools.
In addition, as senior associate dean, Dr. Thomson negotiated several contracts with hospitals in the tri-state area, bringing them into a network of institutions cooperating with the then separate Presbyterian Hospital and New York Hospital.
National Policy Concerns and Leadership
During the 1990s, Dr. Thomson and others became particularly concerned about disparities in health status and health care related specifically to race. “For physicians, the quest for access, equality, and medical justice,” he wrote in an editorial in the Annals of Internal Medicine in 1997, “is in keeping with our professional pledges and responsibilities. Physicians should be the informed, committed, and insistent conscience of such standards.”
Dr. Thomson was elected to the Institute of Medicine, now the National Academy of Medicine, in 1996. He was chair of an academy committee that reviewed and issued a 2013 report, “Examining the Health Disparities Research Plan of the National Institutes of Health: Unfinished Business.”
He co-chaired a panel convened by the Physicians for Human Rights that reported in 2003 on “The Right to Equal Treatment: An Action Plan to End Racial and Ethnic Disparities in Clinical Diagnosis and Treatment in the United States.”
Dr. Thomson’s influence on health care delivery and education has included key leadership positions in professional organizations. He is co-founder and former president of the New York Society of Nephrology and founder and past president of the Association of Academic Minority Physicians. In 1990-1991, he was chair of the American Board of Internal Medicine, the certifying board for the largest specialty in American medicine, after serving for several years as a member of the board producing certifying examinations and policies for internists and internal medicine subspecialties, as well as dealing with salient policy issues including recertification and the introduction of the concept of professionalism in medicine.
 Columbia honored Gerald E. Thomson in 2015 with the inaugural Kenneth A. Forde Diversity Alliance Lifetime Achievement Award. He is pictured with Dr. Forde and other honorees, Linda Aponte-Patel, who received the Faculty Diversity Award; Ashley White-Stern’18, who received the Medical Student Diversity Award; and Iheanacho Obinnaya Emeruwa’14, who received the Resident Diversity Award.
Columbia honored Gerald E. Thomson in 2015 with the inaugural Kenneth A. Forde Diversity Alliance Lifetime Achievement Award. He is pictured with Dr. Forde and other honorees, Linda Aponte-Patel, who received the Faculty Diversity Award; Ashley White-Stern’18, who received the Medical Student Diversity Award; and Iheanacho Obinnaya Emeruwa’14, who received the Resident Diversity Award. Testifying as president of the American College of Physicians before the House Ways and Means Committee in 1995
Testifying as president of the American College of Physicians before the House Ways and Means Committee in 1995 Gerald Thomson, right, with Congressman John Lewis at a 1995 Congressional committee meeting
Gerald Thomson, right, with Congressman John Lewis at a 1995 Congressional committee meetingHe served as president of the American College of Physicians from 1995 to 1996. With an estimated present membership of some 154,000, the national organization of internists is the largest medical specialty organization and second-largest physician organization in the United States. Its mission is to enhance the quality and effectiveness of health care by promoting excellence and professionalism in the practice of medicine. The organization deals with policy issues affecting the delivery of health care, including issues of access to care, universal health insurance coverage, Medicare and Medicaid policy, and, currently, the Affordable Care Act, and provides guidelines for treatment and numerous policy statements.
From 2001 to 2013, Dr. Thomson chaired the board of the Institute on Medicine as a Profession headed by Columbia’s David Rothman. Over the years, IMAP dealt with conflicts of interest and a variety of other issues pertaining to professionalism and inequities in the delivery of health care.
Another pressing ethical concern of the medical profession arose in the wake of the 9/11 terror attacks and Washington’s suspension of the rules of the Geneva Convention in the treatment of detainees in the U.S. war on terror. Dr. Thomson co-chaired an IMAP-Open Society Foundation committee that reviewed physician involvement in the interrogation and torture of U.S. detainees. The committee’s report, “Ethics Abandoned: Medical Professionalism and Detainee Abuse in the War on Terror,” was published in 2014. He also served as a member of the Constitution Project Task Force on Detainee Abuse that published an extensive report in 2013.
 On rounds in 1999 with then third-year students Robert Hauptschein, Sue Kim, and Nicole Jeffrey
On rounds in 1999 with then third-year students Robert Hauptschein, Sue Kim, and Nicole JeffreyClinician and Teacher
Over the years at Harlem Hospital, he presided over daily morning report, had weekly sessions with third-year VP&S students, and held weekly departmental single case reviews and mortality conferences. At the medical center, he rounded on the medical service even while attending to administrative duties, a regular practice he continued several times a year after retirement.
In a profile of Dr. Thomson published in 1999, Deborah Gurner’96 called him a consistent source of guidance and inspiration. “He is a consummate clinician, with the most undeniable manifest diagnostic mastery and a tremendous bedside manner. He’s got a natural charisma.”
Described as an exacting clinician and devoted teacher, he in 2002 was awarded a Columbia Presidential Teaching Award that recognized his teaching. Dr. Thomson himself sums up his career this way: “It all starts with the foundations of being an effective clinician and teacher.”
Editor’s Note: After 31 years as a writer in the alumni office, Peter Wortsman has retired. This is his last profile for Columbia Medicine magazine. Columbia University Press is compiling several of his profiles for an upcoming book.
- Log in to post comments

