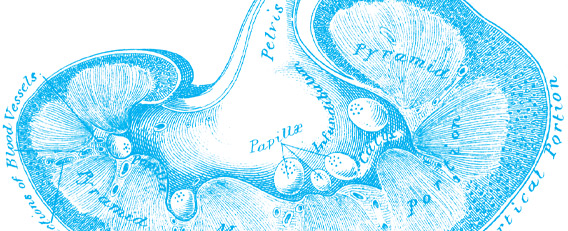
Successful Outcomes Increase Kidney Transplants
Patients in need of a kidney transplant are not only getting them faster at NewYork-Presbyterian/Columbia, they also are living longer than the nationwide average for transplant recipients.
Technical advances developed by surgeon Lloyd Ratner, MD, professor of surgery and director of renal and pancreatic transplantation, have helped make this progress possible.
 ThinkStock
ThinkStockThe first advance, a laparoscopic, minimally invasive surgery for kidney donors, was developed by Dr. Ratner and a colleague in 1995 while they were at Johns Hopkins. At the time, kidney donors faced a more arduous recovery than recipients of their kidneys. Dr. Ratner’s procedure significantly reduced donor recovery times. By making it easier for people to donate kidneys, the number of living donors has increased.
But as more living donors came forward, Dr. Ratner and his team noticed that many intended recipients were incompatible with the donor and produced too many antibodies that were ready to attack the donated organ.
“If a recipient has enough of these antibodies, the recipient could immediately and irreversibly reject the kidney,” Dr. Ratner says.
At that time, two treatments performed before transplantation—plasmapheresis and intravenous immune globulin (IVIg)—were used to try to reduce the number of antibodies in the blood and diminish the chance of rejection. But the success rate of each procedure was only about 30 percent to 40 percent.
In 1998, Dr. Ratner had an idea to combine the two treatments and he devised a protocol that has now become standard practice in the field. “I put the two of them together, and the combination was almost 100 percent successful in reducing the number of antibodies to a sufficiently low level that we could move forward with transplantation,” he says.
In Dr. Ratner’s protocol, the patient first undergoes plasmapheresis, which filters the patient’s blood to remove the dangerous antibodies. Then, IVIg treatment infuses other antibodies into the patient to provide some protection until the immune system regenerates. This desensitization process allows a patient to receive an organ from an incompatible donor.
A compatible organ will always be preferred, but a large percentage of patients waiting for a kidney produce so many antibodies that they will likely never find a match. For these patients, desensitization followed by transplantation with an incompatible kidney improves survival compared to remaining on the wait list, as demonstrated by a recent clinical trial conducted at 22 centers, including Columbia.
Although a 2016 newspaper story described desensitization as a new procedure, Dr. Ratner has been performing it at Columbia since he arrived in 2004. The technique has enabled more than 200 Columbia patients, who otherwise would have remained on the waiting list, to receive kidneys.
Kidney “swaps” also have increased the number of successful transplants in recent years. During a kidney swap, multiple donor and recipient pairs are identified, and donated organs are transplanted into recipients according to compatibility. The strategy allows patients who have a willing but incompatible donor to receive an organ that is a better match than that of their own donor. And, a single donor may be able to help multiple individuals through kidney swaps. Dr. Ratner helped pioneer kidney swaps in 2001 and performed the first kidney swap in New York in 2004.
Despite these improvements, wait times for kidney transplants have continued to rise nationwide. Diabetes, largely driven by the obesity epidemic, is a main reason for the increased need, Dr. Ratner says. “This is a bigger issue than the improvements in transplant techniques. More people are going on the list than the number who get off through transplantation. However, it is important to note that donating a kidney is safer and less intrusive than ever before.”
The transplant team can be reached at 212-305-6469.
- Log in to post comments