Alumni Profile: Karen Kinsell’93

You can still find arrowheads scattered about if you know where to look, trinkets of the Creek War of 1813-1814. Steamboats came and went, carting off cotton and leaving behind an abandoned opera house, a vintage hardware store, a cluster of reconstructed log cabins, and a historic stockade, all faded traces of bygone glory. Once a hub of commerce and a strategic confederate outpost in the War Between the States, Fort Gaines in Georgia today is a picturesque memento of yore on the Chattahoochee River, county seat of Clay County, a three-hour drive south of Atlanta. The county ranked last in the state health assessment for the second year in a row and was designated by the Georgia Office of Rural Health as the most medically underserved county in the state. Fort Gaines’ population of 1,100 comprises 429 households and is roughly 60 percent black and 40 percent white. The town, where the median household income is $18,300, has one doctor.
In fact, the entire county has only one MD tending to the health needs of some 3,600 people: Karen Kinsell’93. Her patient pool includes many destitute individuals, some of whom cross state lines from nearby Alabama to seek care. She regularly works 10-hour days, seeing between 30 and 40 patients, including many uninsured, and charging a nominal $10 a visit “if they can afford it, nothing if they can’t.”
“I have a commitment to the community,” says Dr. Kinsell, who also serves as vice chair of the local school board. “I think I make a difference here. If I left, they would be in pretty bad shape.”
Columbia Medicine shadowed Dr. Kinsell over two days in October 2013 for an interview-on-the-run, conducted in her car, her office, and the local nursing home, where she stopped by after hours to look in on a patient. The patient was close to a century old and weaving in and out of consciousness, but his smile upon seeing Dr. Kinsell said it all.
Practicing “Where They Didn’t Even Know They Needed Me”
A feisty Indiana native not inclined to mince words, Dr. Kinsell, who faced her share of hurdles when she first came to Georgia in 1996 and is still willing to wrangle with the powers that be if the cause is right, says, “I wanted to practice in an underserved area, in a place so ‘sorry’ they didn’t even know they needed me.”
They know. Local feelings for her run strong. “If I could win the lottery, I would build her the finest clinic she ever had,” declares the newly elected Fort Gaines mayor, Tirena Kenyon, who served as Dr. Kinsell’s first receptionist. Absent lottery windfalls and public funding, the doctor makes do with the Clay County Medical Center, in the remodeled, albeit somewhat sagging, premises of a former Tasty Freeze ice cream stand. “It has termites and a tendency to slip into the ditch behind it, but the ceiling holds,” says Dr. Kinsell.
“She’ll drop whatever she is doing to rush to the rescue,” Mayor Kenyon says. “I don’t care where she comes from, these are her people now. She’s one heck of a diagnostician, too, let me tell you. My husband was having severe abdominal pains. It was late at night, so I didn’t want to bother her and took him to the little emergency room in the town next door. Big mistake! After writhing in agony for a day and a half, they told him to go home and take Maalox. I finally called her. ‘It’s his gallbladder,’ she said over the phone after I described the symptoms, ‘get him to the hospital right away.’ He had emergency surgery that afternoon. She saved his life.”
From the Midwest to Midtown, from the Bronx to the Backwoods
A graduate of Lawrence University, a liberal arts college in Appleton, Wis., Karen Kinsell initially pursued a PhD degree in human nutrition at Cornell before switching to a program in geriatric social work at Yeshiva University to have a more immediate impact on people’s lives. After working for seven years as director of two Times Square area residence facilities for homeless women, many with mental health issues, she decided she needed more training and clout to really make a difference; she revived an old idea to become a doctor.
At age 34, having been out of college for 12 years, she buckled down to take the prerequisite premed courses, scored high on the MCATs, and was admitted to several medical schools, opting for P&S “because it was the most rigorous place I got into…and because it offered a dual degree MD-MPH track with the School of Public Health.”
The second oldest member of her class, she was “informed in no uncertain terms that by not starting medical school until age 34 [I] had essentially deprived society of 12 years of being a doctor,” Dr. Kinsell recalls. “I know that it takes tremendous resources to train a physician. And you have a responsibility to do all you can with that education. But I still felt I had a lot to offer. My experiences before medical school helped me tremendously to be a better doctor.”
She enjoyed the patient contact in the clinical years and particularly relished classes in public health, and the combined experience reaffirmed her belief, as articulated by 19th century German physician, pathologist, and public health and social medicine pioneer Rudolf Virchow, that “medicine is politics.”
Among her teachers at P&S, the late Glenda Garvey’69—“Tough! Demanding!”—and pathologist Jay Lefkowitch’76—“Knowledgeable! Cool!”—left indelible impressions. But having decided from the start to pursue a career in primary care while attending an institution that clearly favored specialty training, she admits to having felt “a bit like a fish out of water.” To make matters worse, she fell ill at the end of her second year and had to take a brief leave of absence.
After graduation, Dr. Kinsell pursued training and was chief resident in primary care internal medicine at Montefiore Medical Center and West Central Bronx Hospital, honing her diagnostic skills while treating some of the city’s poorest. “It was grueling and gratifying,” she says, “but there were already a thousand fine doctors floating around in the Bronx, and they didn’t need another.”
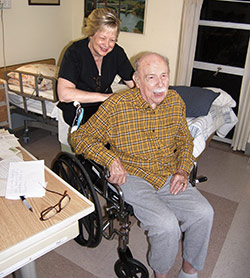 Dr. Kinsell with a nursing home patient
Dr. Kinsell with a nursing home patientAlso, the murder of the Chinese restaurant owner across the street from where she lived gave her pause. That and a bad case of asthma aggravated by pollution and cold made her reconsider city life. “I came from a small Midwestern town but didn’t want to go back there either. I wanted an underserved area where it was warm and I could run around in shirt sleeves most of the year.” She went to the library, got a map and a book of statistics, and considered 10 government-funded clinics for the poor in the Deep South.
She picked a remote corner of Georgia near the Alabama border. But the institutional culture of Albany Area Primary Health Care, an affiliate of Phoebe Putney Health Systems, where she initially decided to practice, did not prove to be a good fit. When her contract was not renewed, Fort Gaines caught her eye as just the sort of place she wanted to practice.
Unsustainable Business Model
Given the current constraints of the American health care system and committed as she is to affordable care, Dr. Kinsell confesses that her business model of charging uninsured patients $10—or nothing—per visit is “financially completely unsustainable.”
She trained to become a certified application counselor under the Affordable Care Act but remains frustrated by the Georgia governor’s refusal to expand Medicaid, which would permit state residents and doctors to benefit from health insurance, despite the state’s large number of uninsured. “Southwest Georgia,” Dr. Kinsell points out, “has the second highest insurance rates in the state, probably a combination of poverty, ill health, and lack of competition, with only one insurer in the region. It would make life a whole lot easier for all if there were a viable payment scheme in place.”
Economics, she points out, is a major factor in medicine. “Poverty causes and complicates so many conditions and diseases. If you’ve had a heart attack, your prognosis if you’re poor is markedly worse. Your ability to afford the medications and take them correctly is compromised. Poverty colors your expectations of what your life should be like. I’ve had young people come in, and when I ask them what they’re going to do, they reply, dead seriously, ‘Either I’m gonna go to auto-body school or else I’m gonna collect my disability.’”
Medical Detective Work
Dr. Kinsell’s patients often present a complex puzzle of interrelated medical, psychological, and social issues. On the afternoon this interviewer sat in on her practice with consent from patients, Dr. Kinsell saw a self-described “germophobe,” a young woman distressed about a lesion on her lip. “The presenting issue was really nothing, but she needed to have her ills acknowledged.” The next patient was a woman who had just had a knee replacement. She complained of being “tired of just sitting there” in a wheelchair, so she got up to walk prematurely and fell. Next came a young man suffering from chronic pancreatitis brought on by alcoholism. He also was diagnosed with bipolar disorder, and the medicine clearly impacted his demeanor. He found and sold precious arrowheads to supplement meager disability payments. Suspecting addiction, Dr. Kinsell was skeptical of his request for additional prescription painkillers.
“A lot of what I do is medical detective work. In most cases you’re not discovering multiple sclerosis,” she says of her day-to-day practice. “Most of it is figuring out how you can treat whatever your patient walks in with in a way that’s actually feasible. And that’s where you need to get clever about how to get people medications they’re not going to be able to pay for.” Her commitment to her patients includes helping them apply for prescription assistance plans with major drug companies. Her abiding concern is: “How do you actually make the care happen?”
Her office walls are decorated with inspirational quotes from Christ, Gandhi, Abraham Lincoln, the Dalai Lama, and others. “It catches people’s attention and helps them and me get through the day. In some respects medical care is very similar to religion,” she says. “You go to see somebody dressed in white robes, in a small room, and you tell them all this private information about yourself. There is something in the human brain, a silent suffering that needs to feel acknowledged. It’s the second oldest profession, OK? Before there was any medicinal arsenal to change the course of biological disease, people still needed to turn to healers, shamans, medicine men. A third of all primary care patients are clinically depressed. Most of the people who came in this morning would not have died if I hadn’t seen them. You’re trying to improve the quality of their daily life.”
The Bitter Side of Sweetness
Having already been interested as a graduate student of nutrition in the adverse effects of sugar consumption, every day Dr. Kinsell witnesses the bitter side of sweetness. Very few of her patients are normal weight. “Obesity causes most diabetes, a lot of hypertension, and, in turn, cardiovascular disease, some cancers, depression, and a lot of arthritis. The number of middle-aged women over 250 pounds with arthritic knees is just overwhelming. People hereabouts will frequently drink a six pack of soda pop and other soft drinks a day. And not just teenagers—mothers and grandmothers, too.
 Dr. Kinsell and a patient
Dr. Kinsell and a patient“I had a vastly overweight lady almost literally run me down with a shopping cart at the Dollar General the other day to tell me how excited she was to lose 20 pounds. She said it took the pressure off her knees, that she could walk again. Her mother, who is likewise obese, was in the hospital with congestive heart failure. Her son, age 15, drinks nothing but soft drinks. I said, ‘You don’t have to buy it for him.’ She said, ‘If we don’t have it, he’ll put sugar in water and drink that.’”
She recalls a day last year when, within 24 hours, three young men came in who were over 400 pounds. “The first was 34 with congestive heart failure. The second was 29 with severe hypertension. The third, age 24, over 430 pounds, came in to address some other issue, but didn’t think he had a problem with weight.
“Of course, lack of adequate education is a tremendous part of the problem. The high school graduation rate among adults is under 58 percent,” she says. Teen pregnancy, drug and alcohol abuse, inadequate asthma prevention, ignorance of basic preventive measures, and the absence of positive role models are among other health issues. As vice chair of the local school board, she has tried to make a modest difference. In recent years she also has written a health column in the local newspaper.
A Job That’s Never Boring
All things considered, she relishes the opportunity to practice primary care medicine the way she wants. In a remote rural practice, “you have to figure everything out for yourself. Well, heck, if I had an X-ray machine, it’d be pretty easy, wouldn’t it? To make an accurate diagnosis without any labs or high-tech equipment, and no second opinion from somebody down the hall, that’s the primary challenge. From a professional standpoint it’s an ongoing test of your medical skills.”
Dr. Kinsell thinks of her practice as “doing Peace Corps work with cable. It may not be as exotic as, say, practicing in sub-Saharan Africa, [but] you’ve got more creature comforts—cable TV, Internet, and such. But what makes the American Deep South any less valuable or worthy or interesting than any other culture?”
Dr. Kinsell has been saluted as a Lions Club “Woman of the Year” and named a National Library of Medicine “Local Hero.” But the real payoff is in the practice. “Would I recommend this kind of lifestyle to others?” she asks. “I like living in a little town and seeing people at the supermarket, seeing what they buy and knowing what they talk about. It helps me be a better doctor. It’s a small enough venue so that you can really make and see a difference. Nothing about this job is ever boring! I don’t have any hospital administrators to second guess what I do. I call all the shots. It’s Disneyland for a doctor,” she adds, before once again reasserting a serious medical mien. “And yes, it’s good to know I’m needed.”
- Log in to post comments

