P&S at 250


1. Which of the following was associated with NASA?
____ George R. Merriam’41
____ Baruch Blumberg’51
____ Charles L. Donaldson’56
____ Story Musgrave’64
2. Which virus causes Kaposi’s sarcoma?
____ Merkel cell polyomavirus
____ human herpes virus 8
____ human immunodeficiency virus
____ hepatitis B virus

3. Which of the following Columbians did not receive a Pulitzer Prize?
____ Walker Percy
____ Siddhartha Mukherjee
____ Robert Coles
____ Robert Butler

4. Whose basic research into the microbiology of a tick-borne epidemic yielded the diagnostic test for rheumatoid arthritis still used by physicians today?
____ Harry Rose
____ Melvin Yahr & Margaret Hoehn
____ Michael Terman
5. Which of the following have been won by Columbians?
____ Emmy award
____ Nobel Prize
____ Pulitzer Prize
____ MacArthur Genius Grant

6. Match these innovations with their innovators.
| forceps | Alvan L. Barach |
| cardiac catheterization | Balbina Johnson & Frank Meleney |
| pediatric heart transplant | James McLane |
| oxygen tent | Eric A. Rose |
| bacitracin | André F. Cournand & Dickinson W. Richards |
7. Which of these addresses have been home to P&S over the years?
____ No. 67 Crosby Street
____ Corner of 23rd Street and Fourth Avenue
____ 3 Barclay Street
____ Duane Street
____ West 59th Street
____ Robinson Street (now Park Place)
____ Magazine Street (now Pearl Street)
8. Who was the first known teacher of a course in pathology?
____ William Osler
____ Alonzo Clark
____ Nicholas Romayne
9. What was the cost for a year of medical school at P&S in 1807?
____ $450
____ $130
____ $290
____ $15
10. For whom is the Atchley-Loeb Conference Room named?
________________________________________________________________________
11. Which members of the early P&S notables had criminal records?
____ Nicholas Romayne
____ William J. Macneven
____ Robert Tucker
12. What was the first official need-based scholarship in P&S?
____ William H. Vanderbilt Scholarship
____ Harsen Prize
____ Alonzo Clark Scholarship
____ Alumni Fellowships
13. Who was the first woman faculty member at P&S?
____ Adelaide Spohn
____ Wera Dantschakoff
____ Rosalie Morton
____ Catherine Coleman
____ Miriam Olmstead
14. What describes the contributions made by P&S psychiatrist Lawrence Kolb?
____ description of phantom limb pain
____ PTSD among Vietnam veterans
____ establishment of the first lithium clinic
15. What is William Stewart Halsted best remembered for?
____ introduction of sterile gloves during surgery
____ as a P&S graduate
____ introduction of radical mastectomy to treat breast cancer
____ as one of the “Big Four” founding professors of Johns Hopkins Hospital
____ addiction to cocaine and morphine
Bonus Question:
Which American university opened in 1821 as Columbian College and whose early medical school graduates are sometimes mistakenly identified as Columbia medical school graduates?
The Answers
1.
All—and most likely others—had a connection to NASA. Story Musgrave, a 1964 graduate and an astronaut for more than three decades, has the most prominent connection. He flew on six space flights. George Merriam, a 1941 graduate, was a consultant to NASA in the 1960s on the possible effects of ion radiation on astronauts. Baruch Blumberg, a 1951 graduate who received a Nobel Prize for the discovery of the hepatitis B virus and development of a vaccine, directed the NASA Astrobiology Institute, dedicated to the study of the origins of life on Earth and the search for life elsewhere. Charles Donaldson, a 1956 graduate, conducted research on weightlessness in space travel for NASA.
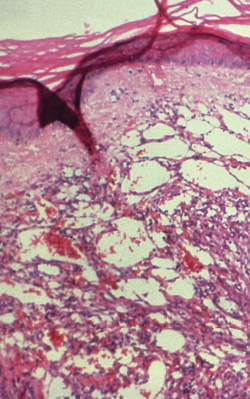
2.
Human herpes virus 8. In the 1980s, doctors treating people infected with HIV began seeing waves of Kaposi’s sarcoma, a rare, slow-growing cancer that often appears as reddish-purple or blue-brown tumors just underneath the skin. By the early 1990s, epidemiologists had begun speculating that Kaposi’s was caused by a sexually transmitted virus, unleashed by the immune suppression triggered by HIV. In 1992, Yuan Chang, MD, then a P&S assistant professor of pathology, and her husband, Patrick Moore, MD, an associate professor of epidemiology, analyzed Kaposi’s sarcoma lesions collected from the autopsy service at Columbia-Presbyterian Medical Center. Using representational difference analysis, which reveals genetic differences in paired biological samples, they identified, in just five weeks, human herpes virus 8, a previously unknown species of herpesviridae. Science published their report in 1994. Now at the University of Pittsburgh, Drs. Chang and Moore subsequently discovered the polyomavirus behind Merkel cell carcinoma.
3.
Even though Walker Percy, a 1941 graduate, received many awards for his novels (“The Moviegoer,” “Love in the Ruins”), he did not receive a Pulitzer. Siddhartha Mukherjee, a faculty member, received a Pulitzer for general nonfiction in 2011 for “The Emperor of All Maladies: A Biography of Cancer.” Robert Coles, a 1954 graduate, received a Pulitzer in 1973, also for general nonfiction, for volumes 2 and 3 of “Children of Crisis: A Study of Courage and Fear,” a series about how children and their parents deal with profound change, including racism and desegregation. He also wrote a popular children’s book based on one child’s experience, “The Story of Ruby Bridges.” Robert Butler, a 1953 graduate, received a Pulitzer in 1976 in the general nonfiction category for his book “Why Survive? Being Old in America.”
4.
Harry Rose. Following a 1946 outbreak of rickettsial pox among residents of Kew Gardens in Queens, P&S chief microbiologist Harry Rose, MD, set out to investigate the chicken pox-like malady with help from Elizabeth Pearce, a young tech in his laboratory. As was not uncommon among researchers in those days, Miss Pearce herself soon developed the disease and thus included samples of her own blood among those she was testing. Among the tests Dr. Rose and Miss Pearce conducted, one measured clotting response. All of the samples tested negative—except that drawn from Miss Pearce, who also had rheumatoid arthritis. Dr. Rose and colleagues at Columbia-Presbyterian’s Faulkner Clinic for Arthritis subsequently observed that more than 50 percent of people with rheumatoid arthritis showed similar clotting responses. The team—with Miss Pearce among the co-authors—reported the findings in the May 1948 Proceedings of the Society for Experimental Biology and Medicine. Years later, it was discovered that, in 1940, Erik Waaler of Norway had reported similar results using sensitized sheep cells, but the discovery had gone unnoticed in the fog of war. Melvin Yahr, the first scientific director of the Parkinson’s Disease Foundation and a pioneer in the development of the amino acid L-dopa as a treatment for Parkinson’s disease, worked with his P&S colleague, Margaret Hoehn, to develop the clinical criteria for Parkinson’s disease that are still used today to evaluate the severity of the disease. Michael Terman, MD, is professor of clinical psychology and director of the Winter Depression Program at the New York State Psychiatric Institute, where his randomized controlled trials throughout the 1990s confirmed the efficacy of bright light as a treatment for seasonal affective disorder.

5.
All of these awards have been earned by Columbia alumni or faculty. Matt Iseman’98 has hosted shows on several TV networks. His hosting of one of those shows, “Clean House Comes Clean,” earned Dr. Iseman an Emmy, a first for the Style network. Other Columbians have received Emmys for health care reporting. Faculty member Siddhartha Mukherjee and alumni Robert Butler and Robert Coles received Pulitzers. Counting current and former faculty, housestaff, MD alumni, and former postdocs and trainees, 22 Columbians with P&S connections have received Nobel Prizes (in physiology or medicine or in chemistry). That includes 2017 Chemistry Nobel Laureate Joachim Frank, a current P&S faculty member. Current faculty member Wafaa El-Sadr and alum Robert Coles have received grants as MacArthur Fellows. Dr. Coles was in the first class of recipients, in 1981.

6.
Forceps: As first director of the Sloane Maternity Hospital, Dr. McLane, an 1864 graduate, designed and used the McLane forceps, later modified as the Tucker-McLane forceps and still used in some deliveries today.
Cardiac catheterization: P&S faculty members André Cournand and Dickinson Richards, a 1923 graduate, were awarded a Nobel Prize in 1956 for their endeavors to reveal the functions of the human heart
and lungs in health and disease.
Pediatric heart transplant: Cardiac surgeon Eric A. Rose, a 1975 graduate, performed the first successful pediatric heart transplant at Columbia during a six-hour operation in 1984.
Oxygen tent: Alvan L. Barach, a 1919 graduate, developed the first practical oxygen tent in the mid-1920s while on the staff of Presbyterian Hospital. Meant for the treatment of asthma, dyspnea, and pulmonary edema, the portable contraption maintained a high percentage of oxygen, while removing excess heat, water vapor, and carbon dioxide.
Bacitracin: A 7-year-old girl, Margaret Treacy, was brought to Presbyterian Hospital’s emergency room in June 1943 for treatment of a leg injury she suffered when she was hit by an automobile. The injury was infected with Bacillus subtilis. A culture taken from the wound was sent to the surgical bacteriological laboratory where its director, bacteriologist Balbina Johnson, discovered that the Staphylococcus aureus seen in the initial microscopic examination had disappeared overnight. Working with surgeon Frank L. Meleney, a 1916 graduate, Ms. Johnson determined that the Staph aureus had been killed by a microbe. Discovery of the microbe led to the development of a powerful new antibiotic. The two named the antibiotic Bacitracin, a combination of parts of the words Bacillus and the child’s surname, which the researchers misspelled as Tracy.
7.
All, except for Duane Street. That’s the address of Rutgers Medical School, established in 1826 when all six members of the P&S faculty resigned to establish a rival institution. While P&S replaced its faculty briskly enough to maintain its educational program uninterrupted, the Rutgers affiliate at Duane Street lasted just four annual sessions. Rutgers would not resume medical education until the 1960s.
8.
Alonzo Clark. Throughout the late 1830s, Dr. Clark, an 1835 graduate, traveled many times to Europe, where he explored methods by which the stethoscope and the microscope might be applied in medical work. When he returned to New York in 1840, Dr. Clark began performing autopsies at New York and Bellevue hospitals, aided by the use of the microscope. He introduced the formal study of pathology as a lecturer at a medical school in Woodstock, Vt. In 1847, Dr. Clark was appointed attending physician at Bellevue, where he introduced the use of the stethoscope for examination of the abdomen and chest. He served as president of P&S from 1875 until 1884. Dr. Romayne, president of P&S from 1807-11, offered the first course in forensic medicine at the Medical Institution of the State of New York, a school he founded after leaving P&S. Dr. Osler, founding physician-in-chief of Johns Hopkins Hospital, authored “The Principles and Practice of Medicine,” a companion to his curriculum for medical education.
9.
A year’s worth of lecture tickets (initially four months) would have added up to $40. With a $5 matriculation fee and room and board estimated at $3-$5 per week, the projected cost for a year of medical school was roughly $130.

10.
Alumni and faculty “of a certain age” will be able to answer this in detail. Dana Atchley (1892-1982) and Robert Loeb (1895-1971) were among the legendary giants of the P&S faculty in the mid-20th century. Drs. Atchley and Loeb (along with other faculty members) moved from Johns Hopkins to P&S in 1921 when Walter Palmer became chair of medicine at P&S. During the 1940s, Dr. Atchley developed the legendary “Atchley History” form, a comprehensive, systematic outline designed to elicit all relevant information from patients about their personal and family histories, prior health and illnesses, and the present illness. His greatest strength, it has been written, was that he urged students to think critically—to weigh evidence, to distinguish fact from fiction in what patients said. Dr. Loeb, who later became chair of medicine, was loved and feared in equal parts. The P&S faculty during the late 1940s and throughout the 1950s had dozens of luminaries, and Dr. Loeb was the star, creating a reputation as a brilliant clinician and bedside teacher. Clinically, he became an expert on Addison’s disease and his team’s pioneering studies of electrolyte abnormalities in human adrenal disease and uncontrolled diabetes made Dr. Loeb and the Department of Medicine world-famous. He is remembered decades later for the indelible imprint he made on generations of medical students, house officers, and members of the medical staff. His first love was teaching students and residents, in whom he inspired respect, veneration, terror, awe, worship, and love.
11.
Romayne and Macneven—as far as we know. Before his appointment as founding president of P&S in 1807, Dr. Romayne was incarcerated for a time in Philadelphia for “high crimes and misdemeanors” associated with conspiracy to gain control of Florida and Louisiana. Dr. Macneven, born in Ireland and trained in medicine at the University of Vienna, was a member of United Irishmen; he was arrested and imprisoned until 1802 for his part in the rebellion of 1798 protesting British rule of the Emerald Isle. In 1770, Dr. Tucker became the first person to be awarded an MD degree by an American college—King’s College Medical School, forerunner of the present-day College of Physicians & Surgeons. Some historians speculate that Dr. Tucker was a British loyalist who fled the Colonies during the Revolutionary War.
12.
The Harsen Prize (1903) was given to second-, third-, and fourth-year students “whose record for ability and scholarship gives evidence of special fitness and who need pecuniary aid to obtain an education.” Third-year student Irving Wilson Voorhees was among the initial recipients. Dr. Voorhees, who graduated in 1905 and became a laryngologist with a specialty in the voice, served 40 years as assistant surgeon at Manhattan Eye, Ear and Throat Hospital and taught for eight years on the P&S faculty. The Vanderbilt Scholarship was among the faculty scholarships created after 1904, a year in which P&S increased tuition by 25 percent. The Alonzo Clark Scholarship was given to faculty “for the purpose of promoting the discovery of new facts in Medical Science.” Alumni Fellowships, created in 1891, were awarded to P&S graduates to support scientific research in anatomy, physiology, or pathology.
13.
The answer depends on how faculty is defined. Per a review by Archives & Special Collections of P&S faculty minutes, several appointments of women were made as early as 1916 but the titles might not qualify them as faculty in today’s use of the term. Adelaide Spohn was named a research assistant in physiology in December 1916. Several of the women listed as possible answers were appointed in 1917 (the same year P&S accepted women students): Miriam Olmstead was appointed as a resident bacteriologist in pathology, Catherine Coleman as a clinical chemist, and Rosalie Morton as an attending surgeon. In 1916, several women were appointed to positions, including assistant physician, in the TB service at Bellevue Hospital, where P&S had a longtime academic affiliation until 1968. The first woman named to a professorial rank at P&S was Wera Dantschakoff, who was appointed an assistant professor in anatomy in March 1917.

14.
All of these and more. By the time Lawrence C. Kolb, MD, arrived at P&S in 1954, he had already crafted the definitive account of the condition now known as phantom limb pain. As chair of the P&S psychiatry department and director of the New York State Psychiatric Institute, he helped to expand psychiatry, integrating it within the medical school and collaborating with politicians and patient advocates to establish mental health clinics in Harlem and other neighborhoods. He advocated for psychiatric care for drug abusers, criminals with mental illness, and those who could not afford it, and he established the nation’s first lithium clinic for the treatment of bipolar disorder. In 1975, he was appointed commissioner of mental health for New York state. His studies demonstrating how combat stress could cause physical symptoms prompted the U.S. government to undertake large studies of post-traumatic symptoms among Vietnam veterans. At Columbia, the research annex to the New York State Psychiatric Institute is named for him.

15.
The answer is subjective, but in terms of medical contributions, William Halsted may best be known for introducing several surgical techniques, notably radical mastectomy. Dr. Halsted’s radical mastectomy was cutting edge in 1882 when he first perfected the technique based on his scientific understanding of the physiology of the breast and his painstaking precision. The procedure became the standard for 75 years. The 1877 P&S graduate is also credited with introducing the use of sterile gloves in the 1890s (because of the dermatitis his surgical nurse Caroline Hampton—later his wife—developed from the carbolic acid solution used to clean the instruments). His mother was his patient in 1882 when he performed the first known operation to remove gallstones. His addiction to cocaine—legal at the time—and morphine was his undoing in New York but he rebuilt his career in Baltimore, where he became one of the founding physicians at Johns Hopkins.
Bonus Question
George Washington University, which opened in 1821 as Columbian College, added a medical department in 1825, the first in Washington, D.C. In 1847, the medical department of Columbian College became the National Medical College, and Columbian College became Columbian University in 1873. The Columbian University Medical School and Hospital were rededicated as the George Washington University Medical School and Hospital in 1904.
- Log in to post comments


